Bilateral CMV Retinitis in a Patient with Relapsed Non-Hodgkin Lymphoma on Oral Metronomic Chemotherapy: Case Report and Review of Literature
CC BY-NC-ND 4.0 · Indian J Med Paediatr Oncol 2025; 46(01): 104-108
DOI: 10.1055/s-0042-1742614
Abstract
Cytomegalovirus (CMV) retinitis is one of the common complications in profoundly immunosuppressed patients such as those with acquired immune deficiency syndrome. It has been rarely reported in patients with lymphoma on aggressive chemotherapy. We encountered a patient with bilateral CMV retinitis who developed this vision-threatening complication while on low-dose palliative metronomic chemotherapy with oral drugs (cyclophosphamide, procarbazine, etoposide, and prednisolone). Though the infection resolved with treatment, there was residual vision loss. This case is presented to sensitize clinicians to the possibility of unusual infections in patients on long-term oral chemotherapies.
Patient Consent
The authors certify that they have obtained all appropriate patient consent forms.
Publication History
Article published online:
26 April 2022
© 2022. Indian Society of Medical and Paediatric Oncology. This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. (https://creativecommons.org/licenses/by-nc-nd/4.0/)
Thieme Medical and Scientific Publishers Pvt. Ltd.
A-12, 2nd Floor, Sector 2, Noida-201301 UP, India
- Cytomegalovirus Retinitis Occurring as a Complication of HyperCVAD Chemotherapy: Report of Two CasesGeetha Narayanan, Indian Journal of Medical and Paediatric Oncology, 2018
- Immune Recovery Uveitis Occurring after Chemotherapy and Ocular CMV Infection in Chronic Lymphatic LeukaemiaY. Wimmersberger, Klinische Monatsblätter für Augenheilkunde, 2011
- Bilateral Cytomegalovirus Retinitis in a 4-year-old Boy with Primary Immune Deficiencyİrem Ceren Erbaş, Klinische Pädiatrie
- Cytomegalovirus Anterior Uveitis from the Perspective of the Common Practitioner: Missed Diagnosis Can Be at the Origin of Severe Functional Loss – A Scenario t...Ioannis Papasavvas, Klinische Monatsblätter für Augenheilkunde, 2021
- Cytomegalovirus Colitis Presenting as a Rectal MassVipul D. Yagnik, Journal of Digestive Endoscopy, 2018
- Neuroimaging of Pediatric Central Nervous System Cytomegalovirus InfectionKathleen R. Fink, Radiographics, 2010
- Cytomegalovirus colitis in AIDS: radiographic findings in 11 patients.E J Balthazar, Radiology, 1985
- Lymphoma of the ConjunctivaMilford D. Schulz, Radiology, 1948
- Case 149: Immune Reconstitution Inflammatory SyndromeKaren C. Chen, Radiology, 2009
- Radiation Therapy for Intracranial LymphomaRobert H. Sagerman, Radiology, 1967
Abstract
Cytomegalovirus (CMV) retinitis is one of the common complications in profoundly immunosuppressed patients such as those with acquired immune deficiency syndrome. It has been rarely reported in patients with lymphoma on aggressive chemotherapy. We encountered a patient with bilateral CMV retinitis who developed this vision-threatening complication while on low-dose palliative metronomic chemotherapy with oral drugs (cyclophosphamide, procarbazine, etoposide, and prednisolone). Though the infection resolved with treatment, there was residual vision loss. This case is presented to sensitize clinicians to the possibility of unusual infections in patients on long-term oral chemotherapies.
Keywords
case report - lymphoma - oral metronomic chemotherapy - cytomegalovirus - retinitisIntroduction
Oral metronomic chemotherapy (OMCT) is often used in patients with relapsed lymphomas. The toxicities of OMCT are generally lower than those of intravenous chemotherapy, making it a preferable option in patients with advanced disease or poor general condition. However, prolonged use of OMCT can lead to immunosuppression and result in unusual infections.[1] Here we describe a rare case of bilateral cytomegalovirus (CMV) retinitis in a patient with relapsed Non-Hodgkin Lymphoma on OMCT.
Case Report
In 2014, a 52-year-old gentleman with no comorbidities with grade 1, stage IV follicular lymphoma achieved complete response after six cycles of rituximab, cyclophosphamide, doxorubicin, vincristine, prednisolone (R-CHOP) chemotherapy. He relapsed in 2017, and lymph node biopsy was suggestive of diffuse large B cell lymphoma. He was treated with rituximab, cyclophosphamide, epirubicin, vincristine, prednisolone (R-CEOP) as he was unwilling for high dose chemotherapy or stem cell transplantation. After five cycles of R-CEOP, he developed a persistent headache. The MRI brain was within normal limits, but the cerebrospinal fluid analysis showed lymphomatous involvement. He was unwilling for any intensive treatment and was started on OMCT with the PEP-C regimen comprising of prednisolone 20 mg once daily for 14 days, etoposide 50 mg once daily for 28 days, procarbazine 50 mg once daily for 28 days, cyclophosphamide 50 mg once daily for 28 days, and triple intrathecal therapy comprising of inj. methotrexate 12 mg, inj. cytarabine 30 mg, and inj. hydrocortisone 15 mg.[2] His symptoms improved significantly after two to three cycles of OMCT. CSF cytology became negative for malignant cells after four cycles of OMCT, and the contrast-enhanced CT scan of the chest, abdomen, pelvis showed no evidence of systemic disease.
In 2019, after 13 courses of PEP-C regimen, he presented with acute onset, painless diminution of vision in both the eyes—right eye (RE) more than the left eye (LE). Visual acuity was hand movements in RE and 6/18 in LE. Fundus examination in both eyes revealed scattered whitish lesions on the retina suggestive of retinitis, along with superficial retinal hemorrhages and perivascular exudates involving the major retinal vessels. The lesions involved the macular center in the RE while the same was spared in the LE ([Fig. 1]). There was no associated vitritis. The differential diagnoses considered were intraocular lymphoma and CMV retinitis. The vitreal aspirate was positive for CMV DNA (deoxyribonucleic acid) PCR (polymerase chain reaction) and negative for malignant cells on cytology. The peripheral blood CMV DNA PCR was positive; however, there were no symptoms of disseminated CMV infection. He had no chest or gastrointestinal symptoms; chest X-ray and LFTs were normal. Thus, there was no evidence of systemic CMV infection. HIV serology was negative. He was managed with intravitreal ganciclovir (2 mg/0.1 mL, weekly once, six doses for each eye) and intravenous ganciclovir (10 mg/kg in two divided doses daily for 1 month). This was followed by oral valganciclovir 900 mg twice daily for 21 days and once daily for 2 months. Gradually, the retinal lesions resolved and manifested healing. CMV DNA PCR of the blood or vitreal aspirate was not repeated, and the disappearance of the retinal vascular sheathing was taken as a marker of clinical improvement. The visual acuity in the RE improved to counting fingers while the LE vision improved to 6/9. OMCT was discontinued as the relapsed lymphoma had shown complete clinical and radiologic response. The patient is currently on follow-up and is alive and well 2 years after the event.
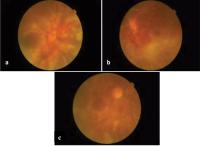
| Fig 1Funduscopic images of both eyes at presentation. Fundus images showing (a) right eye: white retinitis lesions with retinal hemorrhages and perivascular sheathing with involvement of the optic disk and the macula; (b) Left eye: white retinitis lesions with retinal hemorrhages and perivascular sheathing with involvement of infero-temporal retinal quadrant and sparing of the center of the macula; (c) image of the right eye after 2 months showing improvement in retinal hemorrhages and perivascular sheathing.|
Discussion
Our patient had relapsed lymphoma and was on chronic low dose chemotherapy with potential for immune suppression. There were two primary differential diagnoses. One was lymphomatous involvement of the eye, considering the earlier history of meningeal involvement. The second was infectious retinitis, e.g., CMV, toxoplasmosis, candida, pneumocystis, varicella-zoster, and herpes simplex infections.[3] Intraocular lymphoma usually presents as chronic posterior uveitis involving the vitreous (increased haze and cellularity). Additionally, retinitis (perivascular yellowish-white retinal infiltrates and intraretinal hemorrhages) and retinal vasculitis (sheathing of blood vessels) may ensue.[4] CMV retinitis can closely mimic the retinal presentation of intraocular lymphoma.[5] CMV retinitis is seen in 5 to 20%, of patients undergoing solid organ transplantation and in 15 to 30%, of those undergoing allogeneic hematopoietic stem cell transplantation.[6] [7] It presents as focal, perivascular retinal whitening with or without intraretinal hemorrhages and progresses in centrifugal or “brushfire” pattern. It can progress to full-thickness retinal necrosis and retinal detachment.[6] In this patient, the diagnosis was established by detecting CMV DNA PCR of the vitreal aspirate.
CMV serology cannot be used as the sole diagnostic investigation as it can be positive in 80 to 90%, of the general population in India.[8] The gold standard of diagnosis is the isolation of the virus in culture—however, CMV culture is challenging. It takes a long time and is falsely negative in 50%, of cases.[9] [10] On the contrary, DNA amplification techniques (PCR) from blood or vitreal aspirate provide a timely diagnosis with high sensitivity and specificity.[11].[12] CMV retinitis is vision-threatening, and treatment has to be instituted as soon as the diagnosis is established. Intravitreal treatment is vital in vision-threatening disease (central lesions <1 href="https://www.thieme-connect.com/products/ejournals/html/10.1055/s-0042-1742614#JR213170405-13" xss=removed>13] Hence, a combination of intravitreal plus systemic therapy is preferred as was used in our patient. When the disease is not immediately vision-threatening, systemic therapy can be used (IV ganciclovir, IV foscarnet, IV cidofovir, and oral valganciclovir) without intravitreal treatment. Patients are to be monitored with indirect ophthalmoscopy weekly/once in 2 weeks while on induction therapy and monthly till the completion of anti-CMV treatment.[14]
Several cases of CMV retinitis in patients with lymphoma have been described ([Table 1]). Most cases developed in patients on aggressive chemotherapy regimens, which are more likely to produce myelosuppression and immune suppression. Unfortunately, limited data are available regarding risk of CMV relapse while salvaging further relapses. One of the options is to continue chemotherapy with close monitoring of CMV DNA, as is done in the context of an allogeneic transplant. The other option is to avoid immunosuppressive regimens which are heavy on steroids. Our report is the first one describing CMV retinitis during OMCT. The strength of our study is that it highlights that CMV infection is a rare but serious complication of a seemingly less intensive treatment like oral metronomic chemotherapy. The weakness is that we do not have information on the immune status of the patient, like the CD4 counts or immune globulin levels.
|
Sl no |
Author (Ref) |
Lymphoma subtype |
Chemotherapy |
Diagnosis |
Treatment given for CMV retinitis |
Visual outcome |
|---|---|---|---|---|---|---|
|
1. |
Smith[15] |
HL |
MP |
Inclusion body bearing cells (post-mortem) |
NR |
Patient died |
|
2. |
Nasir and Jaffe[16] |
HL |
MOPP-ABVD |
Vitreous biopsy and CMV DNA PCR |
IV gan f/b IV foscarnet |
Improved |
|
3. |
Toy and Knowlden[17] |
HL (R) |
Chl-VPP |
Inclusion body bearing cells (post-mortem) |
Post mortem diagnosis |
Patient died |
|
4. |
Tudesq et al[18] |
HL (R) |
BV |
Vitreous humor aspirate and CMV DNA PCR |
IVtr and IV Gan f/b PO Valgan |
NR |
|
5. |
Tyagi et al[19] |
B-NHL |
R-CHOP |
Vitreous biopsy and CMV DNA PCR |
IVtr and IV Gan f/b PO Valgan |
Improved left eye: Total visual loss |
|
6. |
Kang[20] |
DLBCL |
R-CHOP |
Vitreous aspirate and CMV DNA PCR |
IVtr and IV Gan |
Improved |
|
7. |
Kawai et al[21] |
AITL |
CHOP |
Peripheral blood CMV DNA PCR |
IVtr and IV Gan |
Improved |
|
8. |
Chawla et al[22] |
NHL |
CHOP |
Vitreous biopsy and CMV DNA PCR |
Observation |
Stable disease |
|
9. |
Akpek et al[23] |
NHL |
NR |
Diagnostic vitrectomy and CMV DNA PCR |
IV gan |
Bilateral visual loss |
|
10. |
Vote et al[24] |
PSPL |
Splenectomy, CHOP |
Vitreal aspirate and CMV DNA PCR |
IV gan f/b IV foscarnet |
Stable |
|
11. |
Derzko et al[25] |
DLBCL (R) |
Alemtuzumab, Fludarabine |
CMV DNA PCR of vitreal fluid |
IV gan and foscarnet |
Did not improve |
|
12 |
Reddy et al[26] |
NHL |
Various chemotherapy |
CMV DNA PCR of vitreal fluid |
IVtr, IV Gan and PO Valgan |
Improved |
|
13 |
Current patient |
DLBCL |
PEP-C oral |
CMV DNA PCR of vitreal aspirate |
IVtr, IV Gan f/b PO Valgan |
Improved |
References
- Santos KD, Lien K, Georgsdottir S, Sivanathan L, Emmenegger U. Adverse side effects associated with the use of low-dose metronomic chemotherapy. In: Bocci G, Francia G. eds. Metronomic Chemotherapy: Pharmacology and Clinical Applications. Berlin, Heidelberg: Springer; 2014: 263-279
- Coleman M, Martin P, Ruan J. et al. Low-dose metronomic, multidrug therapy with the PEP-C oral combination chemotherapy regimen for mantle cell lymphoma. Leuk Lymphoma 2008; 49 (03) 447-450
- Guembel HO, Ohrloff C. Opportunistic infections of the eye in immunocompromised patients. Ophthalmologica 1997; 211 (Suppl. 01) 53-61
- Brown SM, Jampol LM, Cantrill HL. Intraocular lymphoma presenting as retinal vasculitis. Surv Ophthalmol 1994; 39 (02) 133-140
- Tang L-J, Gu C-L, Zhang P. Intraocular lymphoma. Int J Ophthalmol 2017; 10 (08) 1301-1307
- Dhillon B. The management of cytomegalovirus retinitis in AIDS. Br J Ophthalmol 1994; 78 (01) 66-69
- Azevedo LS, Pierrotti LC, Abdala E. et al. Cytomegalovirus infection in transplant recipients. Clinics (São Paulo) 2015; 70 (07) 515-523
- Chakravarti A, Kashyap B, Matlani M. Cytomegalovirus infection: an Indian perspective. Indian J Med Microbiol 2009; 27 (01) 3-11
- Shibata D, Martin WJ, Appleman MD, Causey DM, Leedom JM, Arnheim N. Detection of cytomegalovirus DNA in peripheral blood of patients infected with human immunodeficiency virus. J Infect Dis 1988; 158 (06) 1185-1192
- Salmon D, Lacassin F, Harzic M. et al. Predictive value of cytomegalovirus viraemia for the occurrence of CMV organ involvement in AIDS. J Med Virol 1990; 32 (03) 160-163
- Fox GM, Crouse CA, Chuang EL. et al. Detection of herpesvirus DNA in vitreous and aqueous specimens by the polymerase chain reaction. Arch Ophthalmol 1991; 109 (02) 266-271
- Mitchell SM, Fox JD, Tedder RS, Gazzard BG, Lightman S. Vitreous fluid sampling and viral genome detection for the diagnosis of viral retinitis in patients with AIDS. J Med Virol 1994; 43 (04) 336-340
- Jabs DA, Ahuja A, Van Natta M, Dunn JP, Yeh S. Studies of the Ocular Complications of AIDS Research Group. Comparison of treatment regimens for cytomegalovirus retinitis in patients with AIDS in the era of highly active antiretroviral therapy. Ophthalmology 2013; 120 (06) 1262-1270
- Kaplan JE, Benson C, Holmes KK, Brooks JT, Pau A, Masur H. et al. Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from CDC, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. MMWR Recomm Rep Morb Mortal Wkly Rep Recomm Rep 2009; 58: 1-207 ; quiz CE1–4
- Smith ME. Retinal involvement in adult cytomegalic inclusion disease. Arch Ophthalmol 1964; 72 (72) 44-49
- Nasir MA, Jaffe GJ. Cytomegalovirus retinitis associated with Hodgkin's disease. Retina 1996; 16 (04) 324-327
- Toy JL, Knowlden RP. Cytomegalovirus retinitis misdiagnosed as Hodgkin's lymphoma deposits. BMJ 1978; 2 (6149): 1398-1399
- Tudesq J-J, Vincent L, Lebrun J. et al. Cytomegalovirus infection with retinitis after brentuximab vedotin treatment for CD30+ lymphoma. Open Forum Infect Dis 2017; 4 (02) ofx091
- Tyagi M, Ambiya V, Mathai A, Narayanan R. Atypical cytomegalovirus retinitis in non-Hodgkin's lymphoma. BMJ Case Rep. 2015. Accessed June 17, 2021 at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4533632/
- Kang HM. Cytomegalovirus retinitis in patients with diffuse large B-cell lymphoma. J. Retin 2017; 2: 97-100
- Kawai Y, Kawai R, Nakayama T. et al. Successful treatment of cytomegalovirus retinitis in a patient with malignant lymphoma: a case report and review of the literature. Int J Hematol 1999; 69 (04) 256-259
- Chawla R, Venkatesh P, Garg SP, Mandal S, Tewari HK. Cytomegalovirus retinitis in a patient with non-Hodgkins lymphoma: a diagnostic dilemma. Eur J Ophthalmol 2005; 15 (01) 153-157
- Akpek EK, Kent C, Jakobiec F, Caliendo AM, Foster CS. Bilateral acute retinal necrosis caused by cytomegalovirus in an immunocompromised patient. Am J Ophthalmol 1999; 127 (01) 93-95
- Vote B, Russell M, Polkinghorne P. Recurrent cytomegalovirus retinitis in a patient with a normal lymphocyte count who had undergone splenectomy for lymphoma. Retina 2005; 25 (02) 220-221
- Derzko-Dzulynsky LA, Berger AR, Berinstein NL. Cytomegalovirus retinitis and low-grade non-Hodgkin's lymphoma: case report and review of the literature. Am J Hematol 1998; 57 (03) 228-232
-
Reddy S,
Tyagi M,
Behera S.
et al.
Cytomegalovirus retinitis in patients of non-Hodgkin's lymphoma: clinical presentations and outcomes. J Ophthalmic Inflamm Infect 2021; 11 (01) 26
Address for correspondence
Prasanth Ganesan, MD, DMDepartment of Medical Oncology3rd Floor, SSB, JIPMER, Dhanvantari Nagar, Puducherry 605006IndiaEmail: p.ganesan@jipmer.edu.inPublication History
Article published online:
26 April 2022© 2022. Indian Society of Medical and Paediatric Oncology. This is an open access article published by Thieme under the terms of the Creative Commons Attribution-NonDerivative-NonCommercial License, permitting copying and reproduction so long as the original work is given appropriate credit. Contents may not be used for commercial purposes, or adapted, remixed, transformed or built upon. (https://creativecommons.org/licenses/by-nc-nd/4.0/)
Thieme Medical and Scientific Publishers Pvt. Ltd.
A-12, 2nd Floor, Sector 2, Noida-201301 UP, IndiaWe recommend- Bilateral CMV Retinitis in a Patient with Relapsed Non-Hodgkin Lymphoma on Oral Metronomic Chemotherapy: Case Report and Review of LiteratureFen Saj, VCOT Open
- Cytomegalovirus Retinitis Occurring as a Complication of HyperCVAD Chemotherapy: Report of Two CasesGeetha Narayanan, Indian Journal of Medical and Paediatric Oncology, 2018
- Immune Recovery Uveitis Occurring after Chemotherapy and Ocular CMV Infection in Chronic Lymphatic LeukaemiaY. Wimmersberger, Klinische Monatsblätter für Augenheilkunde, 2011
- Bilateral Cytomegalovirus Retinitis in a 4-year-old Boy with Primary Immune Deficiencyİrem Ceren Erbaş, Klinische Pädiatrie
- Cytomegalovirus Anterior Uveitis from the Perspective of the Common Practitioner: Missed Diagnosis Can Be at the Origin of Severe Functional Loss – A Scenario t...Ioannis Papasavvas, Klinische Monatsblätter für Augenheilkunde, 2021
- Congenital cytomegalovirus infection.J M Best, The BMJ, 1987
- Acyclovir for cytomegalovirus infection.P Selby, The BMJ, 1984
- Congenital cytomegalovirus infectionMegan H Pesch, The BMJ, 2021
- Congenital cytomegalovirus infection: a dilemma.M C Timbury, The BMJ, 1984
- A brushfire in the eyeThe BMJ, 2016
- Bilateral CMV Retinitis in a Patient with Relapsed Non-Hodgkin Lymphoma on Oral Metronomic Chemotherapy: Case Report and Review of Literature

| | Fig 1Funduscopic images of both eyes at presentation. Fundus images showing (a) right eye: white retinitis lesions with retinal hemorrhages and perivascular sheathing with involvement of the optic disk and the macula; (b) Left eye: white retinitis lesions with retinal hemorrhages and perivascular sheathing with involvement of infero-temporal retinal quadrant and sparing of the center of the macula; (c) image of the right eye after 2 months showing improvement in retinal hemorrhages and perivascular sheathing.|
References
- Santos KD, Lien K, Georgsdottir S, Sivanathan L, Emmenegger U. Adverse side effects associated with the use of low-dose metronomic chemotherapy. In: Bocci G, Francia G. eds. Metronomic Chemotherapy: Pharmacology and Clinical Applications. Berlin, Heidelberg: Springer; 2014: 263-279
- Coleman M, Martin P, Ruan J. et al. Low-dose metronomic, multidrug therapy with the PEP-C oral combination chemotherapy regimen for mantle cell lymphoma. Leuk Lymphoma 2008; 49 (03) 447-450
- Guembel HO, Ohrloff C. Opportunistic infections of the eye in immunocompromised patients. Ophthalmologica 1997; 211 (Suppl. 01) 53-61
- Brown SM, Jampol LM, Cantrill HL. Intraocular lymphoma presenting as retinal vasculitis. Surv Ophthalmol 1994; 39 (02) 133-140
- Tang L-J, Gu C-L, Zhang P. Intraocular lymphoma. Int J Ophthalmol 2017; 10 (08) 1301-1307
- Dhillon B. The management of cytomegalovirus retinitis in AIDS. Br J Ophthalmol 1994; 78 (01) 66-69
- Azevedo LS, Pierrotti LC, Abdala E. et al. Cytomegalovirus infection in transplant recipients. Clinics (São Paulo) 2015; 70 (07) 515-523
- Chakravarti A, Kashyap B, Matlani M. Cytomegalovirus infection: an Indian perspective. Indian J Med Microbiol 2009; 27 (01) 3-11
- Shibata D, Martin WJ, Appleman MD, Causey DM, Leedom JM, Arnheim N. Detection of cytomegalovirus DNA in peripheral blood of patients infected with human immunodeficiency virus. J Infect Dis 1988; 158 (06) 1185-1192
- Salmon D, Lacassin F, Harzic M. et al. Predictive value of cytomegalovirus viraemia for the occurrence of CMV organ involvement in AIDS. J Med Virol 1990; 32 (03) 160-163
- Fox GM, Crouse CA, Chuang EL. et al. Detection of herpesvirus DNA in vitreous and aqueous specimens by the polymerase chain reaction. Arch Ophthalmol 1991; 109 (02) 266-271
- Mitchell SM, Fox JD, Tedder RS, Gazzard BG, Lightman S. Vitreous fluid sampling and viral genome detection for the diagnosis of viral retinitis in patients with AIDS. J Med Virol 1994; 43 (04) 336-340
- Jabs DA, Ahuja A, Van Natta M, Dunn JP, Yeh S. Studies of the Ocular Complications of AIDS Research Group. Comparison of treatment regimens for cytomegalovirus retinitis in patients with AIDS in the era of highly active antiretroviral therapy. Ophthalmology 2013; 120 (06) 1262-1270
- Kaplan JE, Benson C, Holmes KK, Brooks JT, Pau A, Masur H. et al. Guidelines for prevention and treatment of opportunistic infections in HIV-infected adults and adolescents: recommendations from CDC, the National Institutes of Health, and the HIV Medicine Association of the Infectious Diseases Society of America. MMWR Recomm Rep Morb Mortal Wkly Rep Recomm Rep 2009; 58: 1-207 ; quiz CE1–4
- Smith ME. Retinal involvement in adult cytomegalic inclusion disease. Arch Ophthalmol 1964; 72 (72) 44-49
- Nasir MA, Jaffe GJ. Cytomegalovirus retinitis associated with Hodgkin's disease. Retina 1996; 16 (04) 324-327
- Toy JL, Knowlden RP. Cytomegalovirus retinitis misdiagnosed as Hodgkin's lymphoma deposits. BMJ 1978; 2 (6149): 1398-1399
- Tudesq J-J, Vincent L, Lebrun J. et al. Cytomegalovirus infection with retinitis after brentuximab vedotin treatment for CD30+ lymphoma. Open Forum Infect Dis 2017; 4 (02) ofx091
- Tyagi M, Ambiya V, Mathai A, Narayanan R. Atypical cytomegalovirus retinitis in non-Hodgkin's lymphoma. BMJ Case Rep. 2015. Accessed June 17, 2021 at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4533632/
- Kang HM. Cytomegalovirus retinitis in patients with diffuse large B-cell lymphoma. J. Retin 2017; 2: 97-100
- Kawai Y, Kawai R, Nakayama T. et al. Successful treatment of cytomegalovirus retinitis in a patient with malignant lymphoma: a case report and review of the literature. Int J Hematol 1999; 69 (04) 256-259
- Chawla R, Venkatesh P, Garg SP, Mandal S, Tewari HK. Cytomegalovirus retinitis in a patient with non-Hodgkins lymphoma: a diagnostic dilemma. Eur J Ophthalmol 2005; 15 (01) 153-157
- Akpek EK, Kent C, Jakobiec F, Caliendo AM, Foster CS. Bilateral acute retinal necrosis caused by cytomegalovirus in an immunocompromised patient. Am J Ophthalmol 1999; 127 (01) 93-95
- Vote B, Russell M, Polkinghorne P. Recurrent cytomegalovirus retinitis in a patient with a normal lymphocyte count who had undergone splenectomy for lymphoma. Retina 2005; 25 (02) 220-221
- Derzko-Dzulynsky LA, Berger AR, Berinstein NL. Cytomegalovirus retinitis and low-grade non-Hodgkin's lymphoma: case report and review of the literature. Am J Hematol 1998; 57 (03) 228-232
- Reddy S, Tyagi M, Behera S. et al. Cytomegalovirus retinitis in patients of non-Hodgkin's lymphoma: clinical presentations and outcomes. J Ophthalmic Inflamm Infect 2021; 11 (01) 26


 PDF
PDF  Views
Views  Share
Share

